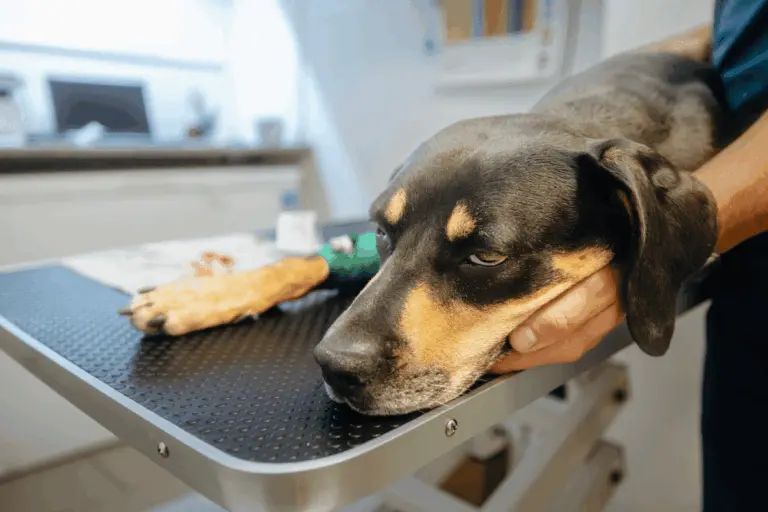
Canine leishmaniasis (known as kala-azar in some places) is a dangerous disease that mainly affects dogs, but can also affect other animals and even humans. It is caused by a parasite called Leishmania, which damages the pet's immune system.
According to the Epidemiological Report on Leishmaniases of the Americas, Brazil registered 12,878 cases of the disease in 2022, with a growing trend between 2023 and 2024. Fiocruz researchers reinforce the warning: the number of infected dogs is also increasing across the country.
In Brazil, almost all cases in dogs are visceral leishmaniasis, caused by the species Leishmania infantum. This is a serious disease that develops slowly and, if left untreated, can lead to the death of both animals and people. It is therefore a major public health problem.
What is canine leishmaniasis?
Canine leishmaniasis is a serious disease caused by a microscopic parasite called Leishmania. This invader enters the dog's body through the bite of an infected mosquito (known as a straw mosquito, birigui mosquito or cangalhinha mosquito, depending on the region).
Once inside the body, the parasite attacks the dog's defense cells and multiplies, spreading to important organs such as:
- Skin (causing sores and scaling)
- Liver
- Spleen
- Kidneys
- Bone marrow
There are two main types of leishmaniasis:
- Cutaneous leishmaniasis - Causes sores on the skin, but is rare in dogs.
- Visceral leishmaniasis - The most dangerous, it affects internal organs and is the one that most affects dogs. Furthermore, in endemic areas, around 40 to 60% of the dogs in an infected population can be asymptomatic.
Why is this worrying?
It's a zoonosis, meaning it can be transmitted to humans (but it doesn't pass directly from dog to person - only via the infected mosquito).
If left untreated, it can be fatal for both animals and humans.
In dogs, the disease is chronic and difficult to control, but with care, it is possible to improve their quality of life.
Symptoms of canine leishmaniasis
Canine leishmaniasis is a tricky disease because many infected dogs show no symptoms for months or even years. When signs do appear, they can vary greatly, as the disease affects several organs.
Main symptoms that the guardian can observe:
Skin problems
- Wounds that won't heal
- Scaling and scabs (especially on the muzzle, ears and around the eyes)
- Hair loss and whitish areas on the skin
Abnormal nails and inflamed paws
- Overgrown nails become thick and brittle
- Cracked or sore paw pads
Weight loss and weakness
- Losing weight for no apparent reason
- Lack of appetite and malnutrition
- Apathetic dog with no energy to play
Fever and swelling
- Persistent low-grade fever
- Enlargement of "lymph nodes" throughout the body
- Enlarged liver and spleen (detectable in tests)
Eye problems
- Red eyes with discharge
- Persistent conjunctivitis
- Excessive blinking or lesions in the area
Bleeding and other serious signs
- Blood in the nose or gums
- Vomiting and chronic diarrhea
- Swelling in the legs (edema) due to kidney problems
Difficulty walking
- Joint pain
- Lameness
Important: Some dogs that are infected show no symptoms, but can still transmit the disease if they are bitten by the mosquito. In regions where leishmaniasis is common, regular check-ups are essential even if the pet seems healthy.
If your dog shows any of these signs, see a vet urgently! The sooner it is diagnosed, the better the chance of controlling the disease.
Transmission of canine leishmaniasis (does it pass to humans?)
Leishmaniasis is not transmitted directly from dogs to people or between animals.
Contagion only occurs through the bite of an infected mosqu ito - in Brazil, the main transmitter is the straw mosquito (Lutzomyia longipalpis).
How does the transmission cycle occur?
- The straw mosquito bites a sick dog (or other infected animal, such as foxes) and sucks blood containing the Leishmania parasite.
- Inside the mosquito, the parasite develops.
- In a new bite, the infected mosquito transmits the disease to another dog or to a human.
Dogs are the main urban reservoirs - The more infected dogs in a region, the greater the risk of transmission to humans if mosquitoes are around.
No direct contact - There's no point in avoiding hugging or kissing your dog: the disease is only spread by mosquito bites.
Can it pass to humans? Yes, but only if a mosquito bites a sick dog and then a person.
Rare cases (out of the ordinary):
- Puppies can be born infected if the mother is sick (vertical transmission).
- Blood transfusion or deep wounds with direct blood contact (very uncommon).
The greatest danger lies with the straw mosquito. That's why protecting your dog with repellents and vaccinations is the best way to prevent the disease in pets and humans.
Diagnosis of canine leishmaniasis (rapid test and examinations)
If your dog shows symptoms of leishmaniasis or lives in an area where the disease is common, it is essential to take him to the vet for specific tests. Early diagnosis increases the chances of controlling the infection and avoiding serious complications.
Main diagnostic methods:
Rapid test (immunochromatography)
It works like a "pharmacy test" - it uses a drop of the dog's blood to detect antibodies against Leishmania.
Result in minutes, useful for initial screening.
Limitation: Can be false negative in recent cases or those with a low parasite load.
Serology (ELISA/RIFI)
It detects antibodies in the blood more accurately than the rapid test.
ELISA and RIFI are more sensitive laboratory tests, used to confirm doubtful results.
Warning: Very early infections may not be detected because the body has not yet produced enough antibodies.
Parasitological examination (cytology/biopsy)
Samples are taken from the lymph nodes, bone marrow, spleen or skin to visualize the parasite under the microscope.
If the protozoan is found, the diagnosis is definitively confirmed.
Challenge: In mild infections, there may not be enough parasites in the sample, leading to a false negative.
PCR (molecular test)
It identifies the parasite's DNA in the blood or tissues, even before antibodies are produced.
More sensitive for early detection, but can also fail if the parasite load is low in the sample analyzed.
No test is 100% foolproof!
Therefore, the veterinarian evaluates:
- Clinical symptoms (sores, weight loss, kidney problems, etc.)
- History of the animal (if it lives or has traveled to risk areas)
- Multiple test results (usually a combination of rapid test + serology + PCR or parasitology)
If there is a strong suspicion, but the tests are negative, the professional can repeat them after a few weeks.
Why is the correct diagnosis so important?
To start treatment as soon as possible and improve the dog's quality of life.
To reduce the risk of transmission, as sick dogs can infect mosquitoes, which then transmit the disease to other animals and humans.
If you notice any suspicious signs, don't wait - see a vet!
Treatment: how to treat canine leishmaniasis
Until a few years ago, dogs with leishmaniasis were unfortunately condemned to euthanasia. This is because the disease has no definitive cure and poses a risk of transmission.
But since 2016, this scenario has begun to change with the release in Brazil of the first veterinary drug authorized for the treatment of canine leishmaniasis: miltefosine (Milteforan®).
The treatment, carried out exclusively under veterinary prescription, aims to control the symptoms and reduce the parasite load in the dog's body, providing a better quality of life and reducing the risk of the animal infecting new mosquitoes. This is called a clinical cure or epidemiological cure - the dog gets better, but the disease is not completely eliminated. For this reason, the dog may relapse and will continue to need monitoring.
Therapy includes:
- Milteforan®(miltefosine): administered for about 28 days;
- Allopurinol: used together to keep the infection under control;
Other medications can be used depending on the dog's condition (such as ointments for the skin or remedies for the kidneys and liver).
Treatment requires commitment on the part of the guardian: regular appointments, examinations, strict control of medication and ongoing mosquito prevention.
Important: even after treatment, the dog is still a carrier of the disease. For this reason, the use of repellent collars and other preventative measures remains essential.
If you're having trouble keeping up with treatment, seek veterinary advice or support from your local Zoonosis Center. Never abandon a sick animal - it depends on you.
Can canine leishmaniasis be cured?
Canine leishmaniasis has no definitive cure, meaning that the parasite remains "hidden" in the body even after treatment. But the good news is that there is a treatment approved in Brazil (with the drug Milteforan®) that can control the disease, alleviate the symptoms and give the dog years of quality life.
Treated dogs can relapse, so they need continuous follow-up with the vet. Even without symptoms, they can still transmit the disease if they are bitten by mosquitoes - so prevention remains essential, even after treatment.
How to prevent canine leishmaniasis
Prevention is the best way to protect your pet from leishmaniasis. The main measures include:
- Vaccine (for healthy and negative tested dogs);
- Repellent collar (keeps mosquitoes away);
- Clean environment (prevents mosquito proliferation);
- Screens and mosquito nets (especially where the dog sleeps);
- Avoid walks at dusk or at night;
- Veterinary repellents and baths with specific products.
Taking care of prevention helps to protect your pet and reduce the transmission of the disease to other dogs and even to humans. In high-risk areas, these measures make all the difference.